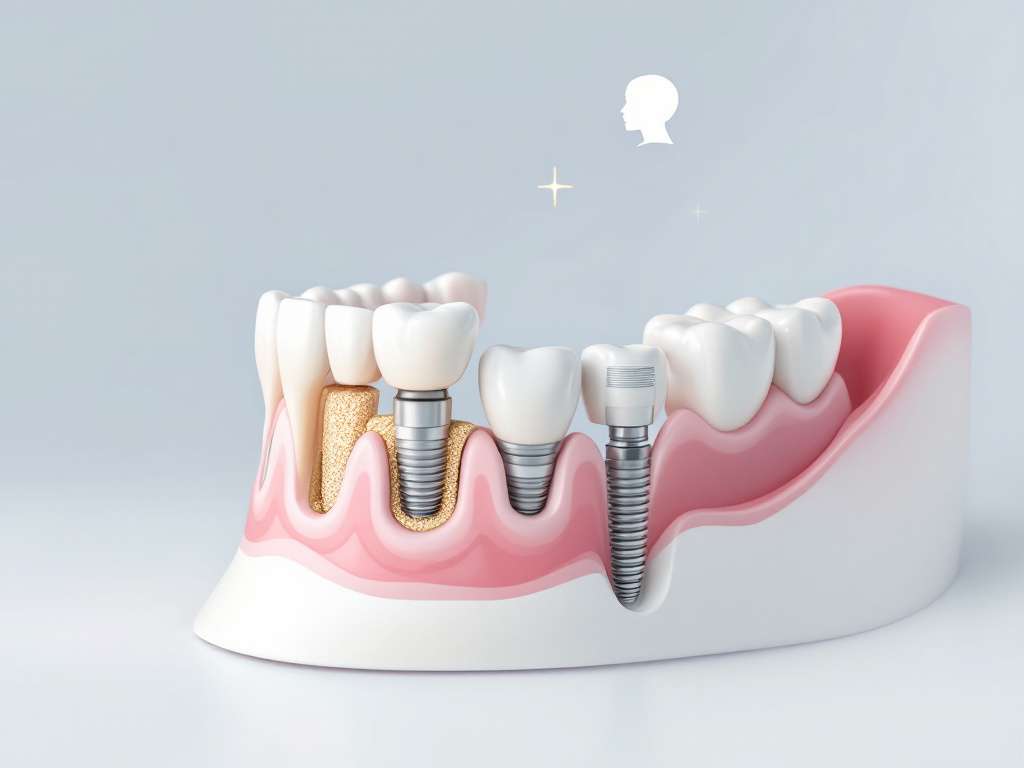
Graft & implant overview
Combining bone grafting and dental implants, also known as graft & implant combination, allows you to rebuild a strong foundation for a healthy, functional smile. When you’ve lost bone volume due to tooth extraction, gum disease or trauma, a graft can restore the jaw’s structure so your implant has the stability it needs for long-term success.
This approach addresses both aesthetic and functional concerns. By augmenting insufficient bone before or during implant placement, you not only improve implant integration but also preserve facial contours and prevent the “sunken” look that often follows tooth loss [1].
“Combining bone grafts with dental implants enhances implant stability and integration, significantly lowering the risk of implant failure or mobility” [1].
Types of bone grafts
You have several options when it comes to graft materials. Each type offers unique advantages and potential drawbacks depending on how much bone you need to rebuild and where the donor material comes from.
| Graft type | Source | Benefits | Drawbacks |
|---|---|---|---|
| Autograft | Your own bone (chin, jaw, hip) | Highest compatibility, excellent success rates | Additional surgery, longer recovery |
| Allograft | Donor human bone | No second surgical site, readily available | Slightly slower integration, minimal rejection |
| Xenograft | Processed animal bone (usually bovine) | Large quantities, preserves space well | Integrates slower, potential for minor resorption |
| Graft extenders | DBM paste mixed with autograft or allograft | Enhances volume, moldable, supports new growth | Cost adds up, careful mixing required |
| Socket graft | Applied immediately after extraction | Preserves ridge shape, simplifies future implants | Limited volume increase, not for large defects |
Planning graft procedures
Before your graft & implant combination, your dentist will perform a detailed clinical examination and imaging study. Cone beam computed tomography (CBCT) helps assess bone volume and quality so you and your provider can decide whether you need a graft and what type suits your situation best [2].
You’ll also discuss timing. If enough native bone remains to anchor an implant, a simultaneous approach can shorten treatment time. Otherwise, a staged plan—graft first, implant later—allows thorough healing over three to six months, maximizing graft success [3].
Sedation options can make complex procedures more comfortable. Whether you prefer minimal sedation for mild anxiety or IV sedation for deeper relaxation, exploring sedation & implant dentistry or iv sedation dental care ensures you remain calm and pain-free throughout your treatment.
Performing graft procedures
Once your treatment plan is set, you’ll return for the graft surgery, often performed in an oral surgery implant clinic setting. Under local anesthesia or sedation, your surgeon exposes the deficient site, prepares the recipient bed, and places the graft material according to the chosen type.
In many cases, your provider will enhance the graft with platelet-rich plasma (PRP) derived from your own blood to boost healing and tissue regeneration [3]. PRP releases growth factors that speed vascularization and new bone formation around the graft particles.
After placement, a protective membrane may be secured to prevent soft tissue ingrowth, and the surgical site is closed with sutures. You’ll receive detailed aftercare instructions and scheduled follow-up visits to monitor healing and address any concerns.
Implant placement timing
Timing your dental implants correctly is crucial for implant success. You have two main pathways:
- Simultaneous placement: If your graft has enough native bone for primary stability, your implant can be placed during the same appointment. This approach reduces your overall treatment timeline and may require fewer surgeries.
- Staged placement: When the deficient area demands larger graft volumes—such as in full-arch restorations or severe atrophy—you’ll wait three to six months after grafting for bone maturation, then receive implants.
For full-arch rehabilitation you might explore an all-on-4 implant procedure or dental implants full arch. In cases where you’re replacing multiple teeth, you could opt for implant supported dentures or a full mouth implant restoration to rebuild both function and aesthetics.
Risks and complications
Every surgical procedure carries some risk. In graft & implant combination, you should be aware of the most common issues:
- Infection at the graft or implant site
- Graft rejection or failure to integrate
- Sinus membrane perforation in upper jaw procedures
- Insufficient bone gain or unexpected resorption
- Implant failure due to compromised stability
Your provider mitigates these risks by adhering to strict sterile protocols, using advanced 3D imaging for planning, and customizing techniques to your anatomy [4]. Smoking cessation, controlling systemic conditions like diabetes, and maintaining excellent oral hygiene also play a major role in preventing complications.
Recovery and aftercare
Your initial healing phase typically spans about a week, during which you may experience mild soreness and swelling. A soft diet, cold compresses and prescribed analgesics will keep you comfortable. Full integration of your graft may take three to twelve months depending on its size and complexity [1].
Once your graft has matured, you’ll receive your implants—ideally within six to twelve months to prevent graft shrinkage [3]. After implant placement, osseointegration generally requires another three to six months before the final implant crown placement or prosthesis.
Long-term success depends on ongoing care. Regular check-ups with your implant and bone graft specialist, diligent brushing and flossing, and possibly adjunctive tools like water flossers will preserve your new bone and implant infrastructure. Explore our guide to implant care and maintenance for tips that help your smile last a lifetime.